As I mentioned on Friday, I gave a webinar last week called “Hockey Hip Assessments: An in-depth look at structural abnormalities and common hip injuries.” Over the last couple years, I’ve become known as a “hip guy”. In reality, I’m not sure how I could train high level hockey players without being a hip guy. Almost half of our players this off-season presented with a hip structure considered “abnormal”, and I think it’s fair to say that every single one of them is flirting with the overuse/under-recovery threshold of their adductor and hip flexor musculature. And these are all “healthy” players. Knowing how to spot individual structure differences and program/coach accordingly is of paramount importance in my setting.
One structural abnormality that is gaining momentum with regards to research attention is femoroacetabular impingement or FAI. I’ve trained several players that have FAI, a couple of which were unaware of their affliction. A 2007 study by Philippon et al. demonstrated that 100% of the 45 professional athletes (24 hockey players) that came to their office with FAI had labral tears. Unfortunately, there is a strong association between labral damage and subsequent osteoarthritis. Recognizing FAI early can help minimize labral damage and the rapidity of osteoarthritis onset, which has the potential to facilitate both short- and long-term performance improvements for the player.
FAI Basics
FAI results in a limitation of hip flexion to around 90 degrees and presents in one of three ways:
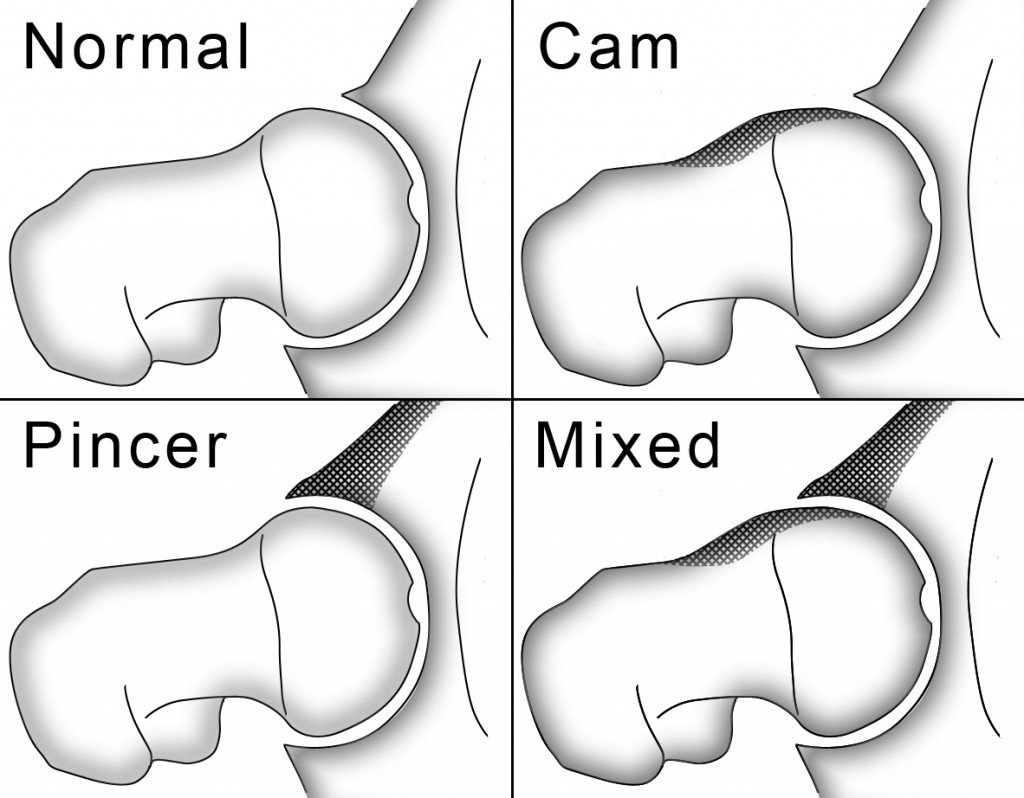
FAI Assessment
Because the common denominator in all forms of FAI is a limitation in hip flexion ROM, you can use a basic quadruped rock to get an idea of whether the athlete has a limitation or not.
Quadruped Rock
Just have the athlete set-up on all fours with their knees under their hips, hands under their shoulders, and spine in a neutral position. Have them push their hips toward their heels while attempting to maintain a neutral spine and note the position of hip flexion that causes a “tucking” of the hips and rounding of the lumbar spine. Ask the athlete where they feel the restriction. If they feel it more in the front/middle part of their hip (“groin” area), it’s more likely a bony limitation than a soft-tissue one. Athletes with FAI will tap out around 90 degrees of hip flexion and feel it primarily in the anteromedial border of their hip.
You can follow up this test by having the athlete lie on their back and take the “suspicious hip” into flexion, adduction, and internal rotation. A significant limitation and/or pain with this movement supports the thought that the athlete has some sort of FAI.
Training Approach
If I suspect an athlete has FAI, we’ll make some very basic adaptations to their training program. Underlying everything we do with these athletes is Mike Boyle’s profoundly simple idea of “if it hurts, don’t do it.” In these cases, I think the athlete’s success has as much to do with what they don’t do, as it does with what they do.
Teach the athlete to perform EVERY movement without flexing the hip past 90 degrees
This is by far the greatest service we can offer these athletes. Every time a player jams through their end range, they put excessive stress on their labrum, and likely cause compensatory problems at neighboring joints. Coaching hockey players with this problem to skate lower or squat deeper will invariably worsen their symptoms and expedite the degeneration process. Range of motion is very individual specific, and these athletes need to be taught how to move within their own structural limitations. This can lead us to making some simple exercise modifications like having the athlete performing 1/2 kneeling exercises with their back knee on a 12″ box to minimize hip flexion of the front leg, and program modifications such as not allowing the athlete to do any lifts off the floor (e.g. deadlifts, trap bar deadlifts, Olympic lifts, etc.).
Favor Single-Leg Exercises
This isn’t a huge change for us because we already place a premium on single-leg training, but it offers the additional advantage for players with FAI of providing more degrees of freedom should the athlete “accidentally” approach hip flexion end range. With bilateral exercises, end range hip flexion is coupled with lumbar flexion, which is an undesirable position for a heavily loaded exercise. In contrast, unilateral exercises allow the hip to tilt in the frontal plane AND usually necessitate lighter external loads, sparing the spine from unnecessary additional stresses associated with compensatory movement.
Augmented Emphasis on Medial Soft-Tissue Work, and Lateral Hip and Posterior Chain Strength/Control Work
Players with FAI tend to have very dense and stiff adductors. Paying extra attention to soft-tissue work to the high adductors, especially where the posterior adductor magnus merges with the medial hamstrings, can help bring some relief to the constant tension these players feel. In theory, the adductors may become overly dense because they adopt a role of tonic stabilizers, functioning to compress the hip joint in an effort to gain stability. Lateral hip work in the form of miniband walks and single-leg exercises can help improve the strength and function of the smaller, dynamic stabilizers of the hip and remove some of this burden from the adductors. Lastly, these players tend to present with an anterior pelvic tilt and poor posterior chain strength. Shifting a greater proportion of their lower body training toward a poster chain emphasis can help restore balance in passive and active strength across the hips.
This is just the tip of the iceberg when it comes to assessing for and training around common hip structural abnormalities. I went into a lot more detail into our assessment and training system in my presentation, which is now available at two of the best strength and conditioning and injury prevention sites out there. If you’re not already a member, I highly recommend you check out Strength and Conditioning Webinars and Sports Rehab Expert.
To your success,
Kevin Neeld
P.S. Both of these sites offer trials for $1. If you’re on the fence, shell out the two bucks and test drive them both to see which may be more appropriate for your needs! Strength and Conditioning Webinars, Sports Rehab Expert
References:
Philippon, M., et al. (2007). Femoroacetabular impingement in 45 professional athletes: associated pathologies and return to sport following arthroscopic decompression. Knee Surg Sports Traumatol Arthrosc. 1597, 908-914.